Endocrine System and Aging: What Changes Over Time
Mar 25, 2026
Aging affects your endocrine system in ways that can influence energy, metabolism, mood, sleep, and overall health. Hormone output and tissue responsiveness change with age, contributing, along with other factors, to muscle loss, weaker bones, slower metabolism, and some cognitive decline. Here’s a quick breakdown of what happens:
- Growth Hormone & IGF-1: Levels drop significantly with age and are associated with reduced muscle repair, lower bone density, and changes in vascular health.
- Sex Hormones: Estrogen, progesterone, and testosterone decline, impacting bone strength, cardiovascular health, and metabolism.
- Thyroid Function: Generally stable with age, although TSH and T3 can shift slightly. In some older adults with mild thyroid dysfunction, this may contribute to fatigue or weight changes.
- Adrenal Aging: Often characterized by higher average cortisol and markedly lower DHEA/DHEAS, and these shifts have been linked to changes in stress regulation and immune function. Evidence for consistent changes in epinephrine with aging is less clear.
- Insulin Resistance: Hormonal shifts increase the risk of diabetes and metabolic issues.
While these changes are natural, lifestyle habits like regular exercise, balanced nutrition, and stress management can help mitigate their effects. Hormone replacement therapy exists, but it’s not always the best option due to potential risks. Observing these changes through hands-on learning, such as cadaver-based studies, provides a clearer understanding of how aging impacts the endocrine system.
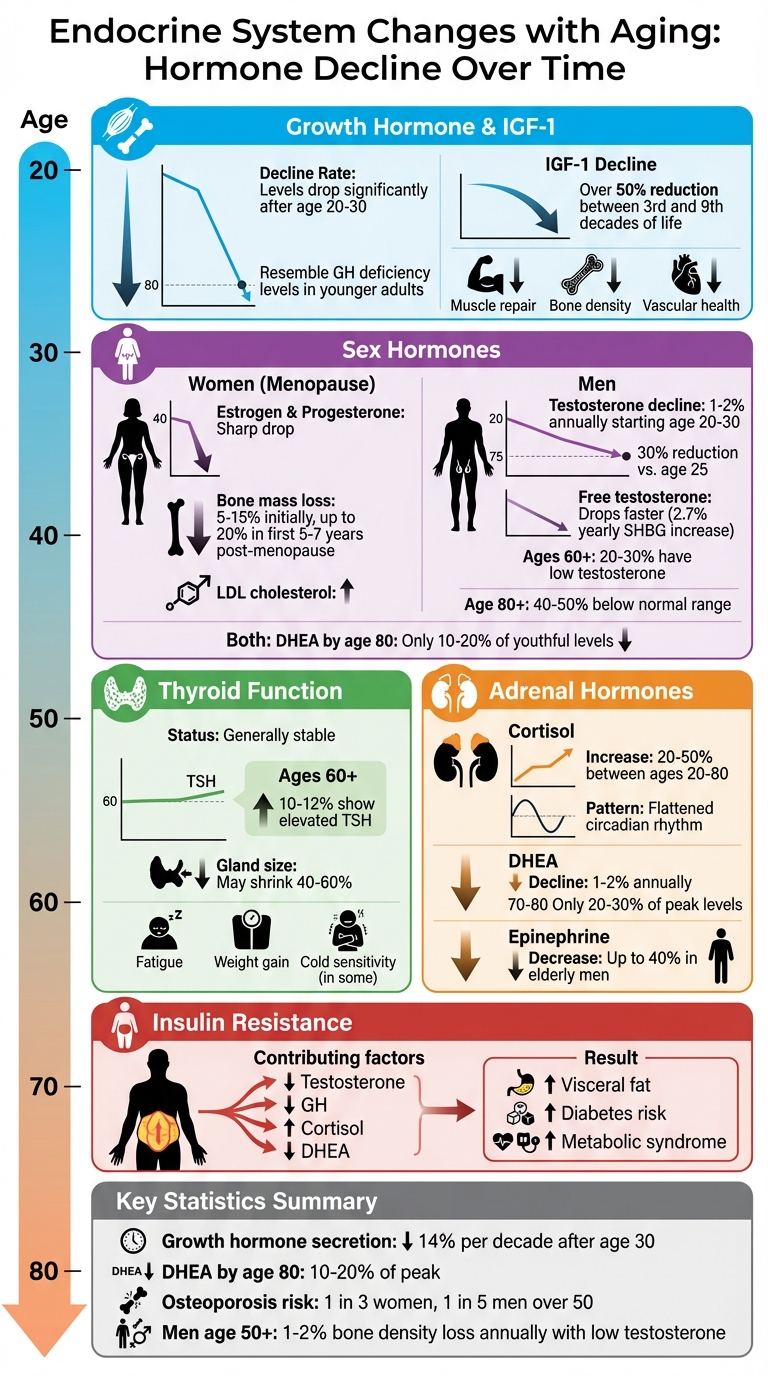
How Aging Affects Hormone Levels: Key Changes by Age
How Does Aging Affect The Endocrine System? - Nursing Knowledge Exchange
Hormonal Changes That Occur with Aging
As we age, shifts in hormone levels play a crucial role in various physical and metabolic changes. Here's a closer look at how specific hormones are affected over time.
Growth Hormone (GH) and IGF-1 Decline
Growth hormone levels begin to drop noticeably after the age of 20 or 30, reaching levels by the eighth decade that resemble those of younger adults with GH deficiency. Similarly, insulin-like growth factor 1 (IGF-1) - a key mediator of GH's effects - declines by over 50% between the third and ninth decades of life.
"IGF-1 is a primary mediator of muscle repair and growth, stimulated by GH in the liver and via its paracrine-autocrine secretion in muscle." – Luis E. Fernández-Garza et al., Researchers
This decline is associated with reduced muscle repair, lower bone density, and changes in vascular health, which may contribute to sarcopenia, osteoporosis, and cardiovascular disease, along with other aging processes.
Beyond growth factors, changes in reproductive hormones also significantly influence aging-related health.
Sex Hormones: Estrogen, Testosterone, and Progesterone
In women, menopause leads to a sharp drop in estrogen and progesterone due to the cessation of ovarian function. This hormonal shift is associated with a 5–15% loss in bone mass in the early postmenopausal years and with adverse changes in blood lipids that may reduce cardiovascular protection.
For men, testosterone levels decline gradually by about 1%–2% annually starting around age 20–30. By about age 75, many men have testosterone levels roughly 20–30% lower than in young adulthood, although this varies widely between individuals. Free testosterone levels drop even faster due to a yearly 2.7% increase in Sex Hormone-Binding Globulin (SHBG), which limits hormone availability. Roughly 20%–30% of men over 60 have low total testosterone levels.
"The anabolic effect of T is reduced during aging due to a gradual and consistent decline in circulating T that begins around the third to fourth decade in men." – Mark W. Pataky, PhD
Both men and women also experience "adrenopause", a steady decline in adrenal androgens like DHEA and DHEAS, which are precursors for estrogen and testosterone. By age 80, DHEA levels drop to just 10%–20% of their youthful levels.
Everything Testosterone Does to Men (And a Little Bit to Women...)
Thyroid Hormone Changes
Unlike growth and sex hormones, thyroid function remains relatively stable with age. Although the clearance of thyroxine (T4) and triiodothyronine (T3) slows down, their production decreases proportionally, keeping serum levels steady in most healthy individuals. While many older adults have slightly higher TSH with normal thyroid hormone levels, a minority develop mild hypothyroidism, sometimes related to autoimmune thyroiditis, which can contribute to fatigue, weight gain, and cold sensitivity in some individuals.
Adrenal Hormones and Stress Response
Aging also affects adrenal hormones, which are critical for stress management. On average, cortisol levels tend to be higher in older adults, and the daily rhythm often becomes flatter, with higher evening levels and a blunted morning rise. Older adults often struggle to shut down the stress response effectively, leading to prolonged cortisol exposure after stressful events.
"Aging is linked to higher mean cortisol levels and reduced sensitivity to negative cortisol feedback." – Maria I. Stamou et al., Maturitas
At the same time, adrenal DHEA secretion declines by about 1%–2% annually, with DHEAS levels dropping to just 20%–30% of their peak by ages 70–80. Additionally, epinephrine secretion decreases by up to 40% in elderly men compared to younger counterparts. Higher cortisol together with lower DHEA in older adults has been associated with greater fatigue, frailty, and altered immune function, which may contribute to increased vulnerability to illness. Evidence for consistent age‑related declines in epinephrine is mixed.
Health Effects of Endocrine Aging
Changes in hormone levels as we age bring about a range of health challenges. As discussed earlier, these shifts can disrupt metabolism, weaken bones, and impair cognitive abilities.
Metabolic Disorders and Insulin Resistance
Hormonal changes, including lower testosterone, reduced growth hormone (GH), higher cortisol, and declining dehydroepiandrosterone (DHEA), play a key role in metabolic issues. Low testosterone is associated with greater visceral fat and reduced insulin sensitivity, which is linked to a higher risk of metabolic syndrome. Reduced GH and IGF‑1 are associated with more visceral fat and less lean muscle, changes that are linked to higher risk of obesity and type 2 diabetes.
Elevated cortisol levels add to the problem by promoting insulin resistance, visceral fat accumulation, and high blood pressure. This creates a vicious cycle: low testosterone and GH contribute to muscle loss, which, combined with reduced physical activity, leads to more fat gain and worsening insulin resistance.
"The commonly observed age-related reduction in insulin sensitivity is likely due to reductions in physical activity rather than aging per se." – Mark W. Pataky, PhD
Testosterone levels drop significantly in men as they age, and in some cohorts, roughly 40–50% of men over 80 have levels below the reference range for younger adults. Fortunately, lifestyle changes like aerobic exercise (five days a week) can improve insulin sensitivity to levels similar to those of younger adults. Resistance training helps counteract muscle loss, and modest caloric restriction (reducing intake to 75–80% of baseline) can further support hormonal balance and insulin function.
These metabolic shifts also weaken bones, making them more prone to damage.
Bone Health and Osteoporosis
The loss of sex hormones as we age directly impacts bone strength. Women, for instance, can lose up to 20% of their bone mass in the first five to seven years after menopause due to the sharp decline in estrogen levels. In men, age‑related declines in testosterone are associated with gradual bone loss, often around 0.5–1% per year after midlife, with higher rates in those with marked hypogonadism.
Osteoporosis is a serious concern, affecting 1 in 3 women and 1 in 5 men over 50. Fractures, a common result of osteoporosis, can have devastating effects. To combat these risks, weight-bearing exercises, along with sufficient calcium and vitamin D intake, are important. Women should consider osteoporosis screenings after menopause, and men with low testosterone may benefit from similar monitoring.
Cognitive and Emotional Health
Hormonal imbalances extend beyond physical health, significantly impacting mental and emotional well-being. On average, cortisol levels tend to increase with age, and higher cortisol is associated with risks for brain health. Research shows that higher morning cortisol levels in patients with early Alzheimer's disease are linked to faster cognitive decline and worsening temporal lobe function.
"In patients with early Alzheimer disease, higher morning plasma cortisol predicts more rapid progression of dementia symptoms and deterioration of temporal lobe function." – Anne R. Cappola, MD, ScM, Division of Endocrinology, Diabetes, and Metabolism, Perelman School of Medicine
In men, lower testosterone levels are associated with a higher risk of memory problems, reduced executive function, fatigue, and depression, although not all studies agree on the strength or causality of these links. Women face cognitive and psychological challenges as well, particularly during menopause when estrogen levels drop. However, the Women's Health Initiative study found that estrogen therapy in postmenopausal women increased the risk of dementia and mild cognitive impairment.
The connection between metabolism and cognition is striking. Older adults with insulin resistance and obesity are significantly more likely to experience cognitive decline. Altered cortisol rhythms, such as higher levels later in the day, are linked to sleep disturbances, which in turn can affect emotional health and mental clarity.
Learning from the Institute of Human Anatomy
Cadaver-based studies offer a fascinating way to explore how aging impacts the endocrine system. The Institute of Human Anatomy provides an immersive learning experience, allowing students and healthcare professionals to observe endocrine glands firsthand and understand their structure and role in the body.
Physical Changes in Endocrine Glands
The structural shifts in endocrine glands align closely with the hormonal declines discussed earlier, highlighting the interconnected nature of endocrine aging. Through cadaver-based learning, these changes become strikingly clear. Take the anterior pituitary gland, for example - it undergoes reduced vascularization and an increase in connective tissue as it ages. This physical transformation correlates with a 50% drop in growth hormone production by the age of 60.
"The structure of the anterior pituitary gland changes as vascularization decreases and the connective tissue content increases with increasing age." – OpenStax
Other glands show similar age-related changes. In older specimens, adrenal glands often show increased fibrous tissue and other structural changes. These changes are clearly associated with reduced production of adrenal androgens such as DHEA, while cortisol and aldosterone production show more variable patterns with age. The thyroid gland can shrink substantially with age in some individuals. When this is accompanied by reduced thyroid hormone output, it may contribute to a lower basal metabolic rate, though many older adults maintain normal thyroid function. Interestingly, while most glands shrink with age, the parathyroid glands often compensate by increasing parathyroid hormone levels to address declining calcium absorption.
These observable changes emphasize the importance of hands-on education, which is a cornerstone of the Institute of Human Anatomy's teaching approach.
Courses and Educational Resources
Seeing these changes in real tissue bridges the gap between theoretical knowledge and practical understanding. The Institute of Human Anatomy offers a variety of learning tools, including interactive courses, videos, and detailed study guides, to bring these concepts to life. Instead of relying solely on diagrams or textbook descriptions, learners can observe real human tissues to better understand endocrine glands and muscle anatomy, and how these relate to functional changes over time.
This hands-on approach not only deepens understanding but also connects the physical transformations of endocrine glands to the hormonal shifts that affect metabolism, bone health, and cognitive function. By making these changes tangible, the Institute equips both students and professionals with a clearer and more practical grasp of endocrine aging.
Conclusion
The endocrine system experiences noticeable shifts as we age, with hormonal changes influencing almost every aspect of health. For example, growth hormone secretion diminishes by about 14% per decade after age 30, while DHEA levels plummet to just 10–20% of their peak by the age of 80. These hormonal declines are associated with muscle loss, increased body fat, fragile bones, and cognitive challenges, alongside other age‑related and lifestyle factors. They also blur the line between normal aging and treatable endocrine disorders, making accurate clinical assessment even more crucial.
While hormone replacement therapy might seem like an easy fix, it’s not a one-size-fits-all solution. Lifestyle changes are generally safer and are strongly recommended as first‑line strategies. Regular aerobic and resistance exercise, combined with adequate calcium and vitamin D intake, can counteract many effects of hormonal aging with far fewer risks than long‑term hormone replacement, which is reserved for specific, carefully selected indications. As Dr. Anne R. Cappola wisely states, "The objective should be to improve health span rather than life span".
"Hormone replacement therapy is not a panacea, as it often results in various adverse events which outweigh its potential health benefits." – Mark W. Pataky, PhD
The structural changes in endocrine glands also tell a compelling story. Observing the physical transformations - like fibrosis in the pituitary or atrophy in the thyroid - provides a clear link between aging and functional decline. Hands-on learning, such as the cadaver-based courses offered by the Institute of Human Anatomy, brings these changes to life. These courses allow healthcare professionals and students to see firsthand how aging alters endocrine function, bridging the gap between academic theory and real-world application.
FAQs
How can I tell normal hormone aging from a treatable disorder?
Normal hormonal aging usually comes with a slow decrease in hormones like growth hormone, estrogen, testosterone, and thyroid hormones. In most cases, these shifts don’t call for medical treatment unless the symptoms become particularly intense. On the other hand, treatable disorders often involve more noticeable issues, such as ongoing fatigue, unexpected weight changes, or challenges with sexual function. Routine medical checkups, including hormone level testing, are key to differentiating between the natural aging process and conditions like hypothyroidism or adrenal insufficiency, which might need medical intervention.
What tests should I ask my doctor for if I suspect hormone changes?
If you think hormone changes might be affecting you, it's worth discussing blood tests with your doctor. Common options include TSH (thyroid-stimulating hormone) tests to evaluate thyroid function, as well as tests for growth hormone and IGF-1, which tend to decrease naturally as we age. These tests can reveal whether your hormone levels are within the expected range or if there are any imbalances that might require further attention.
Which lifestyle habits help most with age-related hormone decline?
To help counter the natural decline in hormones that comes with aging, adopting healthier lifestyle habits can make a big difference. Start with regular exercise, which boosts your body's sensitivity to hormones. Pair that with a nutrient-packed diet to give your body the building blocks it needs for hormone production. It’s also wise to steer clear of smoking and limit alcohol consumption, as both can disrupt hormone balance.
Another key factor? Sleep. Aim for at least six hours of quality rest each night to ease the strain on your endocrine system. And don’t underestimate the power of managing stress - practices like meditation, deep breathing, or yoga can help keep stress hormones in check. Together, these habits support hormonal health and contribute to feeling your best as you age.


