How Overuse Damages Tendons and Ligaments
Apr 23, 2026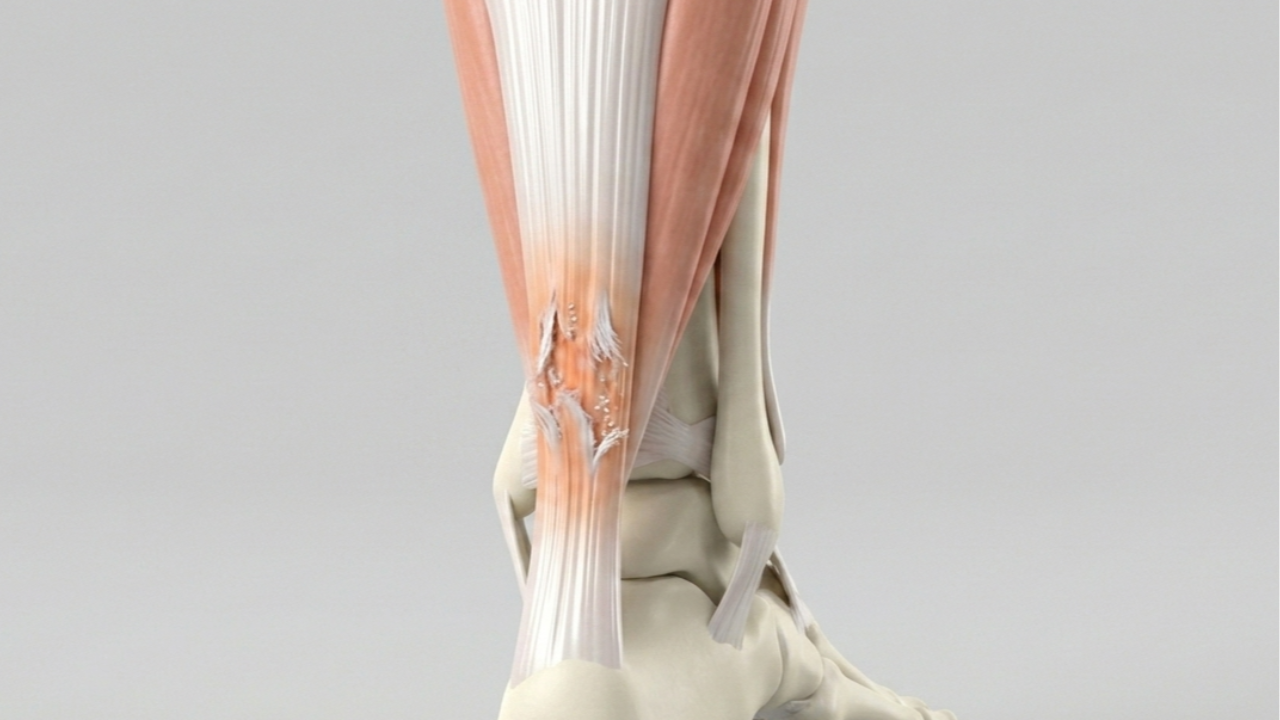
Overusing tendons and ligaments without proper recovery leads to gradual damage. These connective tissues, made of Type I collagen, are strong but heal slowly due to limited blood flow. Repetitive stress causes tiny tears that worsen over time, leading to pain, stiffness, and potential ruptures. Early signs include pain during activity, tenderness, and swelling. Ignoring these can result in chronic injuries, such as tendinosis, which take months to heal and sometimes require surgery. Prevention is key: adequate rest, gradual training increases, proper warm‑ups, and structured rehab exercises (including isometric and eccentric loading) help protect these tissues.
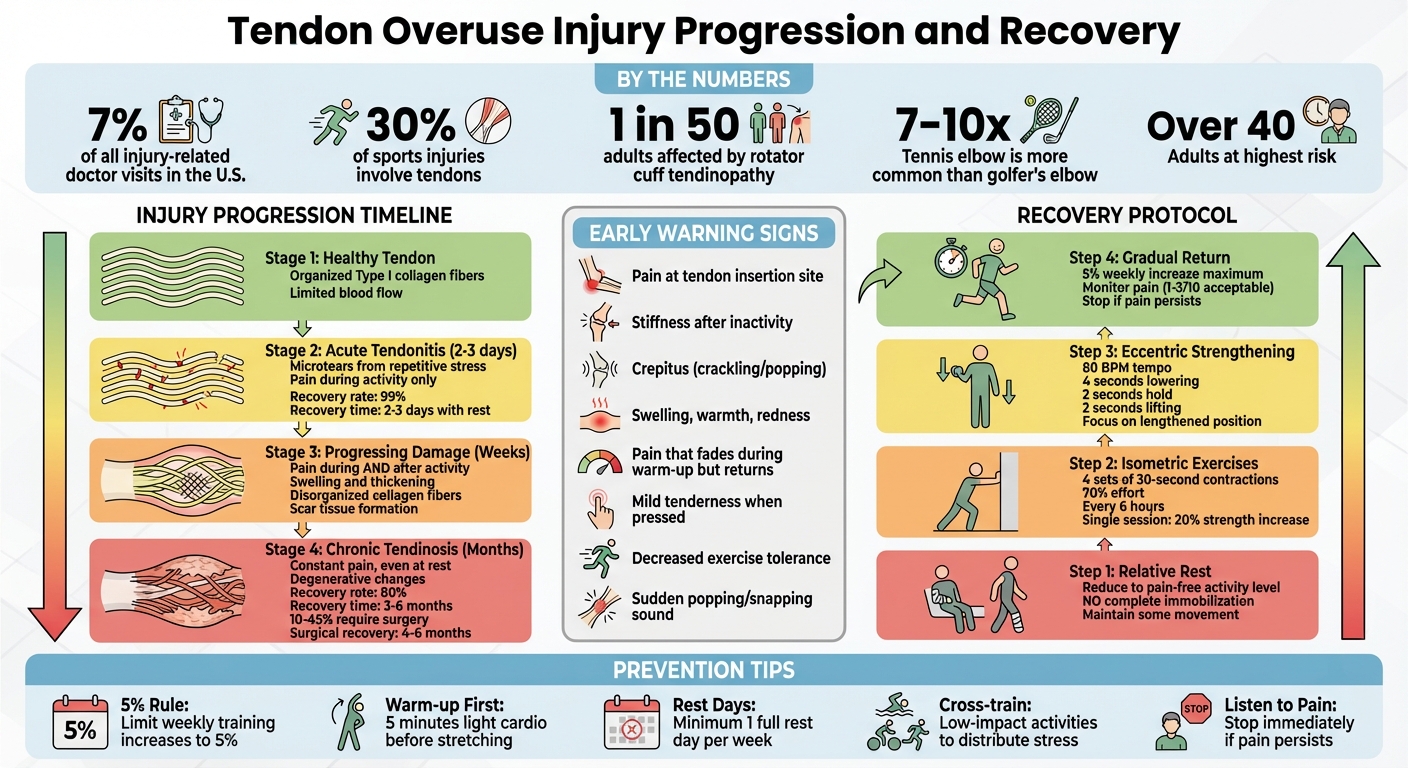
Tendon Overuse Injury Progression Timeline and Recovery Protocol
Symptoms and Early Signs of Overuse Damage
Common Symptoms of Overuse Injuries
Overuse injuries often show up through noticeable physical signs. The most obvious one? Pain at the tendon insertion site. This discomfort usually flares up during or right after activity. As the injury worsens, the pain can shift from a sharp, stabbing sensation during movement to a dull ache that sticks around, even when you're resting. Another telltale sign is stiffness in the affected joint, especially after periods of inactivity.
You might also notice crepitus - that grating, crackling, or popping feeling when you move the affected joint or tendon. Swelling, warmth, redness, and, in chronic cases, thickened or nodular tendons are other visible symptoms.
Overuse injuries are common and account for a substantial share of musculoskeletal and sports‑medicine visits.. Adults over 40 are particularly at risk because tendons lose elasticity and become less resilient with age. For instance, rotator cuff tendinopathy is common in adults, and tennis elbow (lateral epicondylitis) is several times more common than golfer’s elbow (medial epicondylitis).
Early Warning Signs to Watch For
Sometimes, overuse injuries start with subtle clues. One early sign? Pain that fades during a warm-up but comes back as you continue the activity. Dr. David A. Wang, MD, a Primary Sports Medicine Physician at the Hospital for Special Surgery, puts it like this:
"Pain is a way for your body to warn you that something is wrong. Overuse injuries typically begin with a slight pain or discomfort during activity that people ignore."
Another red flag is mild tenderness when you press on the tendon near where it connects to the bone. This is different from general muscle soreness, which is usually more spread out. A drop in your exercise tolerance - when your usual workout suddenly feels much harder - can also point to overuse issues. And if you hear a sudden popping or snapping sound paired with intense pain, it could mean a tendon rupture, which requires immediate medical attention.
Catching these early signs can help prevent minor issues from turning into long-term, chronic problems.
Biological and Mechanical Causes of Overuse Damage
Mechanical Stress and Microtrauma
Repetitive movements can place significant strain on tendons, leading to microtraumas. These tensile forces, especially when excessive, can break down collagen fibers. Uneven strain across the tendon creates areas of stress concentration, particularly near the insertion site where tendons attach to bone. Constantinos N. Maganaris from the Institute for Biophysical and Clinical Research into Human Movement highlights this phenomenon:
"Biomechanical studies indicate that strain patterns in tendons may not be uniform, as tendons show stress-shielded areas and areas subjected to compressive loading at the enthesis."
Interestingly, some parts of the tendon might experience "underuse" despite high overall activity levels, resulting in localized weakness. Other factors like compressive forces during joint movements, heat generated from repeated energy transfer, and the viscoelastic properties of tendons also contribute to ongoing microtrauma. These repeated stresses can overwhelm the tendon’s ability to heal properly, setting the stage for chronic damage.
Biological Failures in Healing
Mechanical stress may trigger tendon damage, but biological factors often prevent adequate recovery. Tendons struggle to repair themselves due to limited blood supply, especially in poorly vascularized areas known as watershed zones. Over time, this lack of effective healing leads to tissue degeneration, with disorganized collagen fibers and weakened structural integrity.
This impaired healing process can lead to chronic tendinopathy (often termed tendinosis), characterized mainly by degenerative collagen changes and typically more challenging to treat than an acute inflammatory episode. In chronic tendinopathy, increased neovascularization and accompanying nerve ingrowth are common and have been linked to persistent pain. Instead of restoring healthy tissue, scar tissue, micro-tears, and calcium deposits often take the place of elastic tendon fibers. For individuals with tendinopathy, the road to recovery can be long and uncertain. In a significant minority of chronic tendinopathy cases, conservative treatments are insufficient and surgery may be considered. Even when healing progresses well, recovery from collagen breakdown typically takes several months.
Progression to Chronic Injuries
From Microtears to Degeneration
When rest is insufficient, tiny microtears in tendons can escalate into more serious issues. Initially, pain only appears during activity. Over time, it becomes constant during exercise and, eventually, persists even at rest. This signals a shift from inflammation to degeneration. Repeated stress without proper recovery leads to swelling and thickening as the tissue struggles to heal properly. Over time, the organized collagen fibers break down and are replaced by chaotic scar tissue, leaving the tendon heavier, stiffer, and weaker. This progression transforms inflammatory tendinitis into degenerative tendinosis.
Timing plays a crucial role in recovery. Mild irritations may improve within days if rest is prioritized, but true tendon injuries require weeks to months for meaningful healing. Chronic degeneration usually requires a much longer treatment period, often at least three to six months of structured rehabilitation.. Recovery outcomes generally decline as problems become chronic: acute tendon problems tend to recover more fully, whereas long‑standing tendinopathy has a lower chance of complete resolution. The American Academy of Orthopaedic Surgeons highlights the risks:
"Persistent inflammation may cause significant damage to the tendon, which may require surgery".
As degeneration worsens, the impact often extends beyond the injured tendon, leading to broader physical challenges.
Compare a healthy achilles tendon with an abnormal (partially torn) achilles
Secondary Problems from Chronic Injuries
When overuse injuries go untreated, the body often compensates by shifting load to surrounding structures, which can alter movement patterns and increase strain elsewhere. Such instability compounds the damage caused by ongoing microtrauma. In young athletes, continuous tension can even lead to avulsion fractures, where the tendon pulls part of the growth plate away from the bone.
The risk of a complete tendon rupture becomes significantly higher with chronic tendinopathy. Similarly, ligament injuries can progress from minor stretching (Grade 1) to partial tearing (Grade 2) and, ultimately, to complete rupture (Grade 3). Boston Children's Hospital underscores the dangers:
"Continuing to play with an overuse injury will worsen the injury, potentially leading to chronic pain, stress fractures, or damage to a tendon or ligament".
In more stubborn cases of tendinopathy, a notable minority of patients may eventually require surgery. Chronic conditions also demand much longer recovery periods. While some acute soft‑tissue injuries may heal over several weeks, recovery after surgery for chronic tendon problems often takes four to six months or more.
Calf Strains, Tendinitis, & Achilles Tears | The Anatomy of the Calves
Solutions: Rest, Rehabilitation, and Prevention
Rest and Recovery Protocols
Skip complete immobilization. While it might seem like a good idea to entirely rest an injured tendon, doing so can lead to muscle weakening and loss of fitness. Instead, experts recommend "relative rest", which involves cutting back on activities to a pain-free level while still maintaining some movement and strength. The American Academy of Family Physicians highlights that "relative rest and reduced activity prevent further damage and promote healing and pain relief".
Recovery times vary widely. Symptoms from a mild, acute tendon irritation may start to improve within a few days with proper rest, but established tendinosis often requires 3–6 months or more of progressive loading and rehabilitation. However, rest alone isn't a complete solution. As Dr. Howard Luks explains: "Rest alone is never sufficient. Tendons need load to remodel and regain capacity". This means controlled exercises must be gradually reintroduced to strengthen the tendon.
Rehabilitation Techniques
Once relative rest has been established, structured rehab exercises play a key role in recovery. Many protocols start with heavy isometric contractions (for example, several 30–45‑second holds at about 70–80% effort), performed regularly through the day, under professional guidance. These exercises can help relieve pain in many people and contribute to the progressive loading that supports tendon adaptation. Research suggests that sufficient time under tension is important for stimulating tendon cells, but the exact ‘optimal window’ is not firmly established. Some studies show that a single session of prolonged isometrics can meaningfully reduce pain and temporarily improve strength, although responses vary between individuals and tendon types.
As pain diminishes, you can move on to eccentric strengthening exercises, which focus on the lengthening phase of movement. To maintain proper tempo, use a metronome set to 80 beats per minute: 4 seconds for lowering (eccentric phase), 2 seconds for holding, and 2 seconds for lifting (concentric phase). This method improves tendon strength and mechanical properties, and some studies suggest it can partially reverse degenerative changes in chronic tendinopathy. Include exercises that load the tendon in more lengthened positions, which may provide additional benefit when integrated into a comprehensive program.
Prevention Through Activity Modification
Tweaking your activities can help not only with recovery but also with avoiding further tendon strain. A useful rule of thumb is to increase weekly duration or distance only gradually (for example, by no more than about 5–10% per week), to reduce the risk of overuse injuries. Dr. Emily Harold from the University of Utah Health explains: "It's so painful that almost no one does it [increasing mileage by 5%], which is why we see a lot of tendon injuries". The American College of Sports Medicine also advises keeping increases in training volume between 2% and 10% per week to reduce the risk of overuse injuries.
Warm up before stretching. Spend 5 minutes on light cardio - like brisk walking, easy jogging, or cycling - to get your heart rate up and prepare your muscles. Save stretching for after your workout when your muscles are already warm and more flexible. Pay attention to your pain levels during exercise: as long as discomfort stays mild (around 1 to 3 on a 10‑point scale), eases during or after activity, and does not worsen the next day, continuing training is generally acceptable. If pain escalates, reduce load or seek advice. However, if tendon pain becomes persistent, stop the activity immediately and use ice to help reduce inflammation.
These adjustments, combined with proper recovery strategies, can help reduce the chances of recurring injuries from overuse.
A Runner’s Guide to Tendon Injuries
Conclusion: Protecting Your Tendons and Ligaments
Overuse injuries don’t happen overnight - they build up over time due to repeated stress and inadequate recovery. Understanding how these injuries develop and why healing can fail is crucial for preventing long-term damage. To put it in perspective, tendon injuries account for a significant portion of musculoskeletal complaints, and more than a third of sports injuries in some groups involve tendons.
The importance of early action can’t be overstated. Addressing tendon issues promptly greatly improves the chances of full recovery, whereas long‑standing tendinopathy has a lower likelihood of complete resolution. Recovery times vary widely, from a few weeks for minor acute problems to 3–6 months or longer for chronic tendinopathy. As Dr. Emily Harold, a Sports Medicine Specialist, emphasizes:
"Once you have them, tendon injuries can take a long time to improve so it's really better to prevent them from happening in the first place".
Preventing tendon injuries boils down to a few key practices: gradual progression, proper rest, and good technique. For example, limit training increases to small, gradual steps (often no more than about 5–10% per week), take at least one full rest day each week, and always warm up before starting any activity. Adding low-impact cross-training can also help distribute stress and reduce repetitive strain. These precautions become even more essential after age 40, as tendons lose elasticity and become more prone to tearing.
Pay attention to warning signs. Persistent pain during or after activity is often a red flag for a worsening injury. If this happens, stop what you’re doing, apply ice, and seek professional advice before continuing. Your tendons are essential for every movement you make - protect them with smart training, proper rest, and careful recovery.
FAQs
How can I tell tendon pain from normal soreness?
Tendon pain caused by overuse often comes with symptoms like tenderness, a protective reflex known as guarding, or even unusual sensations such as popping or clicking. Unlike typical soreness, which usually settles within a day or two, tendon pain often worsens with ongoing use and may not fully resolve with rest alone.
When should I stop training and see a doctor?
If you experience ongoing or worsening pain, swelling, tenderness, or signs of injury that persist for three to six months without improvement, it's time to stop training and consult a doctor. Don't wait if the symptoms are severe enough to disrupt your daily life - seek medical attention right away.
How do I return to exercise without re-injuring my tendon?
To prevent re-injury, it's important to stick to a gradual, load-focused rehab plan. Begin with gentle isometric exercises and gradually move on to strength-loading as your tendon adjusts. Be cautious about sudden jumps in intensity, and keep an eye on pain levels - any exercise should only cause mild discomfort at most. Recovery often takes around 3 to 6 months with proper care, including controlled loading and avoiding overuse, though some cases may take longer. If you're unsure, consider consulting a healthcare professional for a personalized approach.


