Blood Clots: Silent Signs, Risks, and Prevention
Apr 13, 2026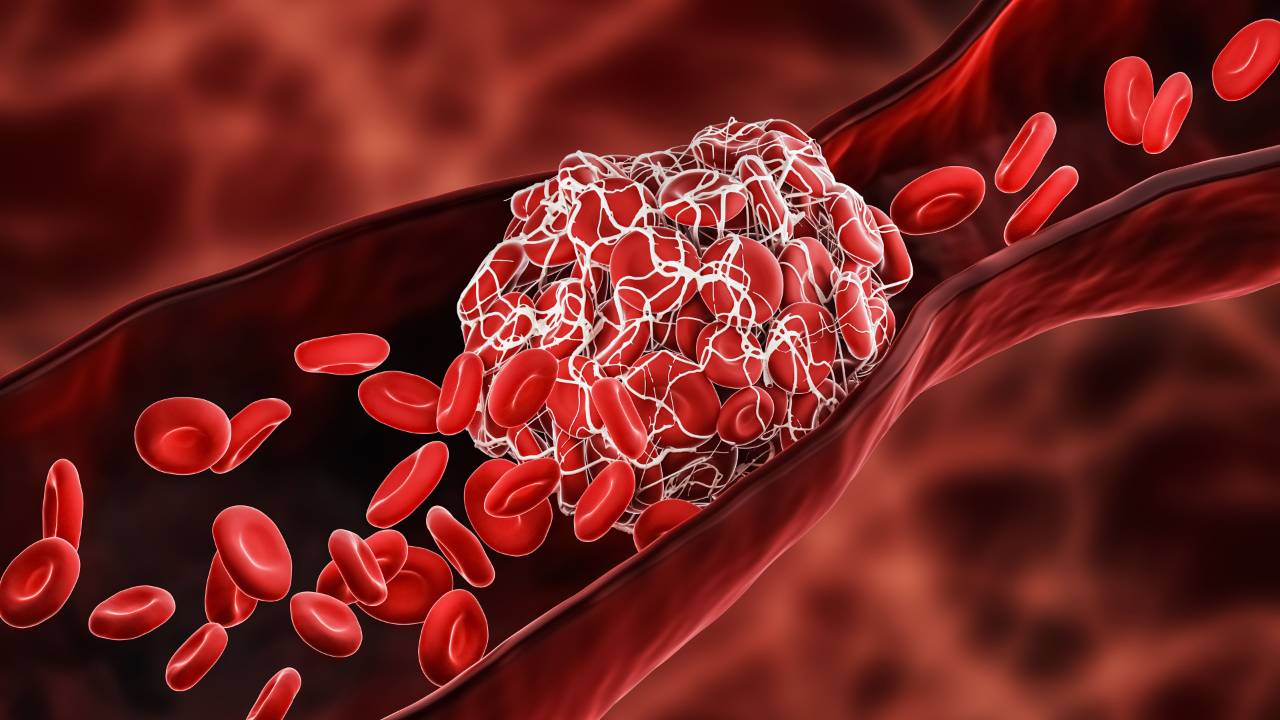
Blood clots, though often overlooked, can have serious and sometimes life-threatening consequences if not identified and managed promptly. In this article, we’ll explore the science behind blood clots, the symptoms to watch for, and strategies to reduce your risk. Using the personal story of a pulmonary embolism survivor as a lens, we’ll dive deep into this critical topic to empower you with the knowledge you need to stay healthy.
What Are Blood Clots and Why Do They Form?
Blood clots, or thrombi, are masses of blood components that aggregate in a specific location. While essential for stopping bleeding (a process called hemostasis), clots can occasionally form abnormally within intact blood vessels, leading to a condition called thrombosis. Understanding the basic components of blood clots can help unravel their dual role in both healing and harm.
Components of a Blood Clot:
- Platelets: Small cell fragments that become sticky and aggregate at sites of vessel injury or abnormal surfaces.
- Red Blood Cells: Trapped within the growing clot.
- Fibrin: A protein that forms a mesh-like scaffold, stabilizing the clot.
While hemostasis is life-saving and stops excessive bleeding, thrombosis is dangerous because it creates blockages in blood flow, leading to potential complications.
Arterial vs. Venous Clots: Key Differences
Blood clots can form in either arteries or veins, and each type presents unique risks:
Arterial Clots:
Arteries, responsible for delivering oxygen-rich blood to tissues, can develop clots that block oxygen and nutrients, resulting in tissue death. This often leads to severe outcomes such as:
- Stroke: A clot in the brain's arteries (e.g., the middle cerebral artery) can deprive brain tissue of oxygen, causing severe damage.
- Heart Attack: A blockage in the heart's arteries (e.g., the left anterior descending artery) cuts off oxygen to cardiac tissue, leading to heart muscle death.
Venous Clots:
Venous clots, commonly forming in the legs or pelvis, can grow large and are often less immediately noticeable. They can cause complications such as:
- Deep Vein Thrombosis (DVT): A clot in the deep veins, often accompanied by pain, swelling, warmth, or redness in the affected limb.
- Pulmonary Embolism (PE): If a piece of a venous clot breaks off (becoming an embolus) and travels to the lungs, it can block blood flow, causing chest pain, shortness of breath, and sometimes cardiovascular collapse.
DVT and Pulmonary Embolism: A Dangerous Duo
Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE) are interconnected conditions that can have grave consequences. Venous clots often form silently due to slower blood flow and the presence of collateral venous pathways. However, they become dangerous when they dislodge and travel through the circulatory system.
How Pulmonary Embolism Happens:
- A clot forms in the deep veins of the leg or pelvis.
- The clot travels upward through larger veins into the inferior vena cava and the right side of the heart.
- The clot is pumped into the pulmonary arteries, where it becomes lodged, blocking blood flow to the lungs.
PE reduces oxygenation, places immense strain on the right side of the heart, and can lead to heart failure or death. Common symptoms include:
- Sudden chest pain
- Shortness of breath
- Rapid heart rate
- Lightheadedness
In severe cases, PE is a medical emergency requiring immediate intervention.
What You NEED to Know About Blood Clots...
Risk Factors for Blood Clots
Several factors can increase the likelihood of blood clots forming. These include both lifestyle-related and medical causes:
- Immobility: Long periods of inactivity (e.g., during surgery recovery, long flights, or car rides) can cause blood to pool in the veins.
- Surgery and Trauma: Major surgeries, especially pelvic or orthopedic procedures, increase clotting risk due to tissue injury.
- Pregnancy and Hormonal Therapy: Hormonal changes elevate clotting potential.
- Smoking: Damages blood vessels and increases clotting risks.
- Genetic Clotting Disorders: Certain inherited conditions predispose individuals to abnormal clotting.
Case Example: The video recounts the story of a woman who developed a pulmonary embolism after undergoing pelvic surgery. The surgery, combined with immobility during recovery, created the perfect conditions for clot formation.
Prevention: How to Reduce Your Risk
While it’s impossible to eliminate all risks, there are practical steps to lower your chances of developing dangerous clots:
- Stay Active: Regular movement, especially during long periods of sitting, helps maintain healthy blood circulation.
- Follow Post-Surgical Care Instructions: Take prescribed medications, wear compression stockings, and move as soon as it is safe after surgery.
- Recognize Warning Signs: Seek medical attention for unexplained pain, swelling, or redness in a limb.
- Address Lifestyle Factors: Quit smoking, maintain a healthy weight, and stay hydrated.
- Be Aware of Family History: If you have a family history of clotting disorders, discuss preventive strategies with your healthcare provider.
The Role of Early Intervention in Saving Lives
Pulmonary embolism is a medical emergency, but early recognition and treatment can significantly improve outcomes. Treatment often involves:
- Anticoagulants (Blood Thinners): Medications that prevent further clot formation and allow the body to break down existing clots.
- IVC Filters: Devices placed in the inferior vena cava to catch clots traveling toward the lungs.
- Lifestyle Adjustments: Continued mobility and adherence to long-term care plans reduce future risks.
The story shared in the video illustrates the importance of acting swiftly. The individual’s family history and recognition of symptoms - chest pain and shortness of breath - prompted immediate medical attention, ultimately saving her life.
Key Takeaways
- Blood Clots Serve a Dual Role: While essential for stopping bleeding, clots become dangerous when they form abnormally inside blood vessels.
- Arterial vs. Venous Clots: Arterial clots starve tissues of oxygen, while venous clots, like DVT, can travel to the lungs and cause pulmonary embolism.
- DVT and PE Are Silent but Deadly: Many clots form without symptoms, making prevention and awareness critical.
- Risk Factors Are Manageable: Regular movement, avoiding smoking, and following medical advice post-surgery are effective ways to reduce risks.
- Act Fast for Pulmonary Embolism Symptoms: Sudden chest pain, shortness of breath, or rapid heart rate requires immediate medical attention.
- Prevention is Key: Staying active, recognizing warning signs, and addressing lifestyle factors can significantly lower your risk.
Understanding how blood clots form, recognizing their potential dangers, and taking preventive steps are critical for safeguarding your health. By being proactive and informed, you can reduce the likelihood of experiencing these life-threatening complications.
Source: "The Silent Warning Signs of Blood Clots" - Institute of Human Anatomy, YouTube, Mar 1, 2026


